On this page
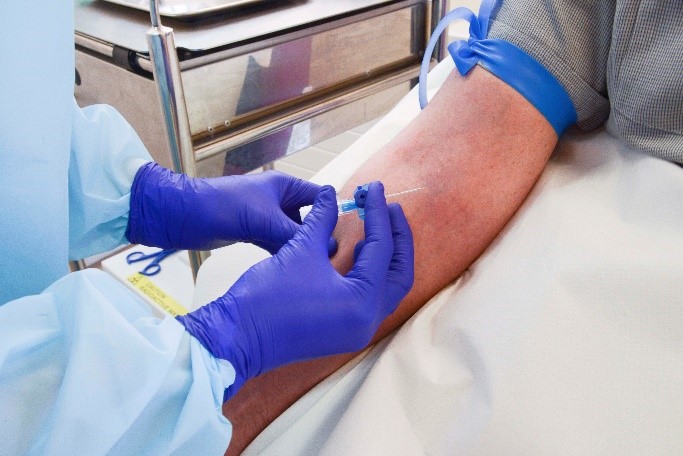
Most nuclear medicine tests involve patients having a small amount of radioactive liquid injected into a vein in their arm or hand. Some studies don’t require an injection – you may be asked to consume some radioactive food and drink instead.
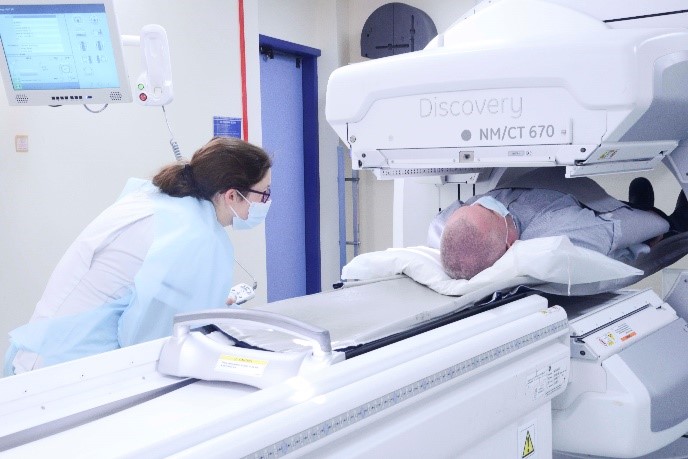
This is followed by one or more pictures being taken of the relevant body part; for this, patients usually lie down on our camera bed. The cameras are often very close to you, but don’t touch you and they are not noisy. Depending on the test you are referred for, you may find that we do 3D pictures with the cameras moving slowly around you, or we may ask you to stand up for the pictures.
We have three nuclear medicine cameras (gamma cameras) in our department, two of which can perform CT scans to supplement our images, which helps our doctors with their diagnosis.
The Nuclear Medicine team also manufacture’s Krypton-81m gas, a ventilation agent used to check lung function.
Radiation Doses in Nuclear Medicine.
Nuclear medicine investigations all involve a small radiation dose, like when you have X-rays taken, or a CT scan. We check all referrals carefully to ensure that you only undergo tests that are necessary to help diagnose (or in a few cases, treat) your condition. We aim to ensure that the benefits of the test outweigh the very small risks from the procedure.
We all receive background radiation doses every day. We are exposed to radiation in the food we eat, the air that we breathe and cosmic rays coming from space. The amount of radiation we receive each year will vary – people who take lots of flights or live in certain parts of the country will receive higher levels than others.
Diagnostic nuclear medicine procedures give too small a dose to give immediate harmful effects such as radiation sickness. At such low levels, the only known possible effect is a slight increase in overall lifetime cancer risk, but this may not be apparent for many years or even decades later.
In the UK our average radiation dose is 2.2mSv, but it varies between 1.5mSv and 7.5mSv, depending on where you live. Many of our tests give additional radiation doses below or around these levels. To put the risks into perspective, the lifetime risk of dying from cancer is 25 per cent, having the most common nuclear medicine heart scan increases that to 25.04 per cent. For other tests, this can be even less. For example, our lung scan which looks for a blood clot known as a pulmonary embolism, the risk rises from 25 per cent to 25.01 per cent. Common examination doses can be found here: https://www.gov.uk/government/publications/medical-radiation-patient-doses/patient-dose-information-guidance.
Women attending Nuclear Medicine will be asked to confirm they are not pregnant or breastfeeding before we continue with your appointment. For people who are breastfeeding, it is wise to call into the department in advance of your appointment as we are able to advise whether you will be asked to stop breastfeeding for a short period of time after your visit to us. One of our tests is commonly performed in pregnant patients, but in some cases, we would reschedule until after delivery of your baby.
Protective equipment
You will see our staff wearing gloves, aprons and visors whilst giving you your injection. You may also notice that the syringe itself is encased in a metal shield. This is to protect us – if you were our only patient that day, we’d be able to handle your injection without the protective shield with very little risk to ourselves. Because we are handling radioactive products many times each day, we need to take extra precautions, including ensuring we don’t accidentally get the radioactive liquid on our skin and uniforms.
Specific patient group information
Children
Children are more sensitive to the effects of radiation because they are still growing, and their cells are dividing rapidly. To keep the doses received by children to a minimum, they will need to be weighed when they arrive in the department. This allows us to administer the correct amount of our injection, in proportion with their size. One parent is welcome to stay in the room with their child for both the injection and scan, and there is usually no need to remove any clothing. They will need to lie still for the images: for younger babies and toddlers, we encourage parents to ensure the child is tired at the time of imaging in the hope that they will sleep whilst we take the pictures. For those that are not yet toilet trained, we’ll give you advice on how to safely dispose of used nappies – they’ll contain trace amounts of radioactivity as your child clears it from their system. If your child is two or over and you’d like us to use numbing cream for their injection, please arrive one hour before your allocated appointment time.
Elderly
For elderly patients, the radiation risk from nuclear medicine tests is actually smaller, so don’t worry if you find yourself having several different types of scans in a small space of time. If you are particularly uncomfortable lying flat, then you might wish to bring some painkillers with you to your appointment – we can advise you when to take them, so they are working well when we are ready to do your imaging. If you need someone to support you because you may be hard of hearing or struggle with memory for example, then you can bring someone with you to your appointment. At busy times, they may be asked to wait in a separate area after your injection. If you suffer with incontinence, let one of our staff know – we’ll give you advice on where/when to store any used pads or catheter bags.
Claustrophobic patients
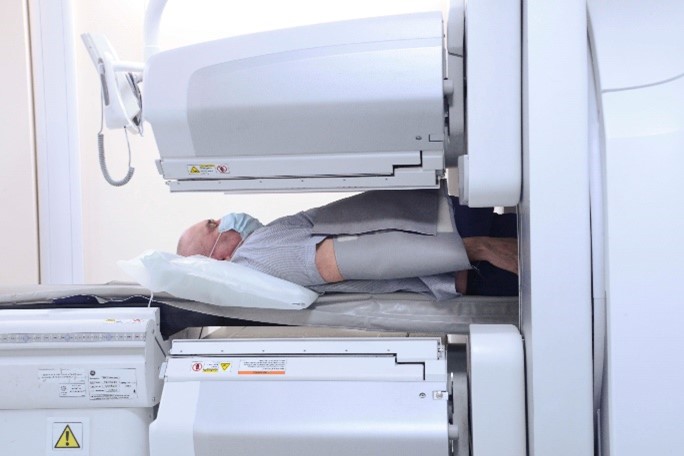
The image shows an example of how our cameras will be quite close to you (they may be in a different orientation or over a different part of your body). If you are worried, let us know when you attend. We’ll discuss how we may be able to keep the camera a little further away (your images won’t be quite as good) and show you how open the cameras are at the side. We’ll do our best to put you at ease and your get your pictures done.
After the scan
For most of our tests, you’ll be able to return to work/home and continue with your normal routine – you shouldn’t feel any ill-effects from the appointment. Depending on the procedure you’ve had with us, we may ask you to avoid long periods of close contact with pregnant people or small children, but this is usually just for the following 24 hours.
Your images will be analysed after the scan, prepared by our clinical technologists or clinical scientists so that they are ready to be viewed by our doctors. The report that is generated will then be sent to your referrer – this is often a hospital doctor rather than a GP. This can take up to two weeks and we advise you to contact your referrer if you don’t receive any information about your results.
Specific information about the test you need will be included in your appointment letter. Additional general information about nuclear medicine can be found at https://www.bnms.org.uk/page/PatientsCarers. For any unresolved queries, please call us on 0121 507 4427.
Patient Information
For more information about disabled access for this service